The healthcare staffing industry change we’re witnessing today marks one of the most significant shifts in modern healthcare operations. With the Joint Commission’s recent updates to its Accreditation 360: The New Standard, the industry is entering a new era of accountability and transformation. For the first time, nurse staffing has been formally recognized as a National Performance Goal, emphasizing that safe patient care depends directly on sufficient, qualified, and well-managed nursing staff.
These new regulations are pushing healthcare organizations to rethink how they approach recruitment, retention, and workforce management. In a landscape already challenged by high turnover and burnout, especially in behavioral health and emergency care, ensuring adequate staffing is no longer optional. Facilities that fail to meet these expectations could risk losing accreditation, compelling leaders to adopt flexible workforce strategies like per-diem staffing and to leverage healthcare staffing automation tools that streamline scheduling and compliance.
As hospitals and agencies adapt to this healthcare staffing transformation, technology is becoming the backbone of sustainable change. From AI-driven scheduling to predictive analytics and automated credentialing, innovation is reshaping how the industry attracts and manages talent. In short, these evolving standards are not just regulatory updates; they represent a fundamental transformation of the healthcare staffing workforce, setting the stage for a smarter, more resilient future.
A New Standard That Puts Nurse Staffing Front and Center
Since 1951, The Joint Commission has been the gold standard for healthcare quality across the United States. Its accreditation system currently recognizes over 20,000 organizations and programs that contribute to high-quality patient outcomes. In fact, most states rely on this major nonprofit as part of their licensing and certification requirements, making its standards a cornerstone of hospital operations.
Now, a significant healthcare staffing industry change is underway. For the first time, nurse staffing has been included as a National Performance Goal, part of a broader initiative called Accreditation 360: The New Standard. This comprehensive update aims to make the accreditation and certification process more streamlined, transparent, and data-driven for healthcare facilities.
Key highlights of this update include:
- Goal 12 of Hospital National Performance Goals: Hospitals must ensure they are staffed adequately to meet patient needs, and that staff are fully competent to deliver safe, high-quality care.
- Leadership responsibility: Hospital leadership is now required to prioritize staffing across all departments, ensuring the workforce is qualified, balanced, and resilient.
- Nurse executive oversight: A licensed registered nurse (RN) will now direct and oversee nursing staffing and operations, ensuring the hospital’s workforce aligns with patient care demands.
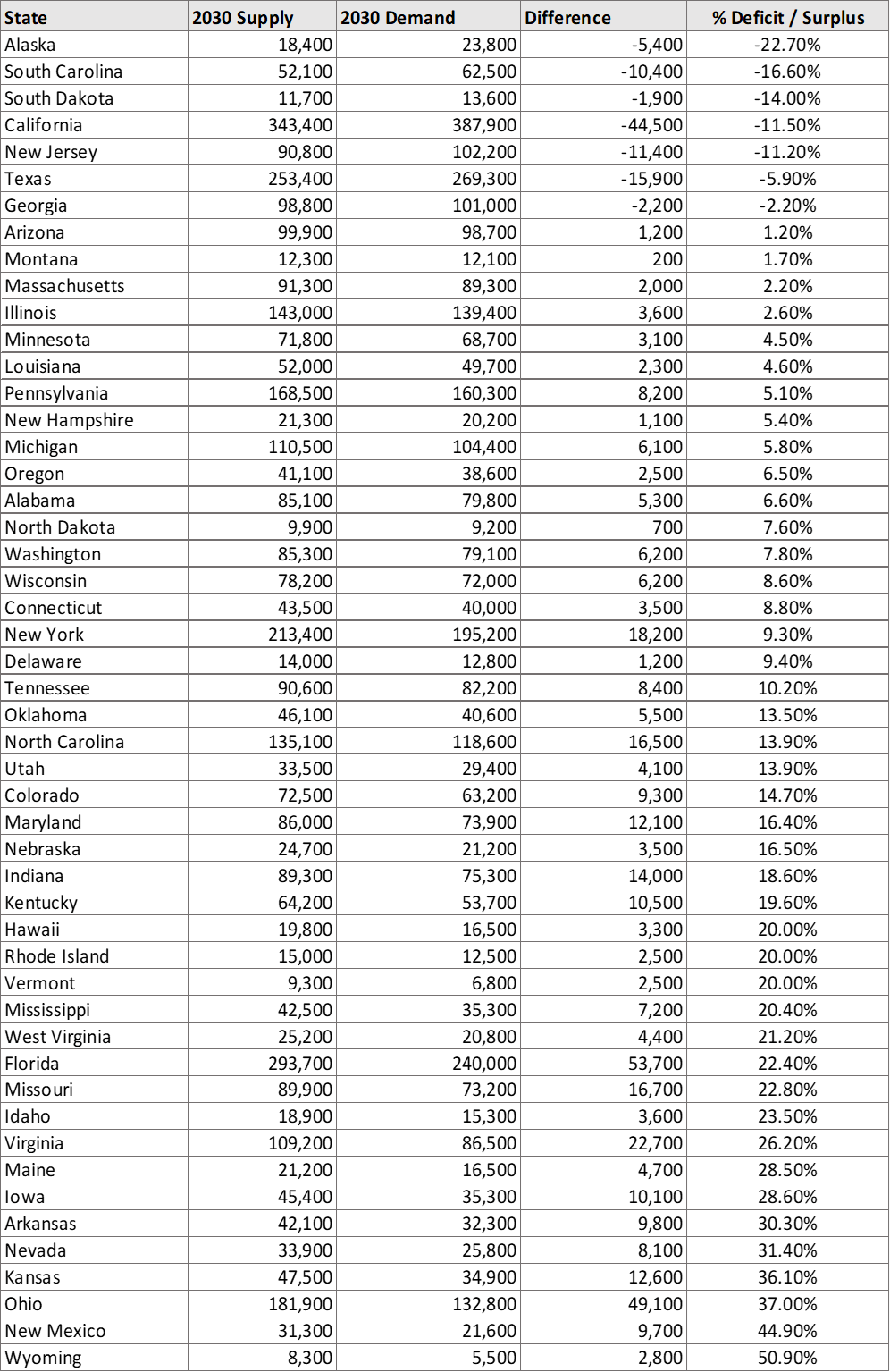
To maintain accreditation, hospitals must now document and demonstrate how they plan to achieve and sustain adequate staffing levels. Many facilities are turning to healthcare staffing workforce technology and data-driven models that factor in departmental patient needs to ensure compliance and optimize care delivery.
Why Nurse Staffing Matters
Even though the updated standards do not prescribe strict nurse-to-patient ratios, making nurse staffing a performance measure sends a clear signal about its importance. Proper staffing is now central to:
- Recruitment and retention: Attracting and keeping skilled nurses is crucial, particularly in high-turnover areas like behavioral health and emergency services.
- Reducing burnout: Adequate staffing helps nurses manage workloads, improving job satisfaction and reducing burnout.
- Optimizing workforce management: Hospitals can leverage healthcare staffing automation tools to better schedule staff, monitor shifts, and balance workloads.
- Improving patient care: Higher staffing levels mean patients receive more attention, experience fewer complications, and often enjoy shorter hospital stays.
Ultimately, by emphasizing nurse staffing as a National Performance Goal, the healthcare staffing transformation is not just about compliance; it’s about creating a more resilient, efficient, and patient-focused workforce.
Other Changes with Accreditation 360
The Joint Commission’s update goes beyond staffing. Key transformations include:
- Streamlining requirements: Over 700 outdated or redundant standards have been removed, including rules like smoking-related policies, which are now largely unnecessary.
- Greater transparency: Hospitals and the public now have online access to updated standards, improving visibility and accountability.
- AI integration: Recognizing the role of technology in modern healthcare, The Joint Commission is collaborating with the Coalition for Health AI to establish guidelines for the safe and ethical use of AI. This includes:
- Streamlining clinician workflows
- Delivering personalized patient care
- Ensuring ethical and compliant AI applications
- Streamlining clinician workflows
These updates signal a larger healthcare staffing industry change, where technology, workforce optimization, and automation converge to enhance both hospital workforce management and patient outcomes.
How Hospitals and Clinics Can Prepare for 2026
As hospitals and healthcare facilities look toward 2026, preparing for the upcoming healthcare staffing industry change is essential. Meeting new standards requires strategic workforce planning, and one of the most effective ways to achieve this is through per-diem staffing.
Per-diem staffing allows hospitals and clinics to bring in skilled professionals on a shift-by-shift or day-by-day basis, making it easier to:
- Cover peak periods: Ensure patient care is never compromised during high-demand times.
- Fill gaps quickly: Provide immediate coverage for absent staff or unexpected surges in patient volume.
- Support specialized procedures: Bring in professionals with the right expertise exactly when and where they are needed.
Beyond addressing immediate staffing needs, per-diem models also help hospitals manage workforce costs more effectively. Facilities can scale operations based on demand, avoiding overstaffing during slower periods while maintaining quality care.
Additionally, adopting per-diem staffing supports a more focused approach to workforce management. Hospitals can:
- Streamline nurse staffing and scheduling
- Optimize employee training and onboarding
- Implement healthcare staffing automation tools for efficient shift planning and compliance
- Improve overall hospital workforce management by using data-driven insights to predict staffing needs
By leveraging these strategies, healthcare organizations can not only meet the new Joint Commission standards but also create a more agile, resilient, and satisfied workforce. This proactive preparation is a critical part of the healthcare staffing transformation taking shape in 2025 and beyond.

How Staffing Standards Are Shaping Opportunities for Nurses and Healthcare Job Candidates
For healthcare professionals, especially nurses, the recent healthcare staffing industry change introduced by the Joint Commission brings new opportunities. As hospitals and clinics work to meet updated standards, there is an increased demand for qualified nursing staff, creating a wider array of job openings that often come with greater flexibility in shifts, responsibilities, and compensation.
To take full advantage of these opportunities, job-seeking candidates should consider the following:
- Update your resume and credentials: Ensure your experience reflects the service areas where you have expertise. Hospitals are particularly interested in skills relevant to patient care, such as infection prevention, surgical services, or pharmacy experience.
- Highlight versatility and experience: Facilities need a workforce with a mix of skills and experience to meet diverse patient needs. Showcasing specialized competencies can make you more attractive to potential employers.
- Explore flexible roles: With per-diem and other flexible staffing models, nurses may find opportunities that align better with their lifestyle and career goals.
The new Joint Commission standards aren’t just about staffing numbers; they’re designed to improve workflow for nurses and other clinicians. By streamlining accreditation requirements and reducing administrative tasks, nurses can spend less time on paperwork and more time on patient care.
This shift is part of a broader healthcare staffing transformation, supported by hospital workforce management and healthcare staffing automation tools. Some of the benefits include:
- More time for patient-focused care during shifts
- Enhanced training and orientation opportunities
- Streamlined workflow, allowing clinicians to focus on outcomes rather than documentation
- Increased job satisfaction and reduced burnout
In essence, these updated staffing standards are designed not only to ensure compliance but also to empower nurses to do what they entered the profession to do: care for patients effectively and safely. By aligning workforce strategies with these changes, hospitals can create a more resilient, efficient, and satisfied healthcare workforce.
Creating Positive Change in Healthcare Staffing
The Joint Commission’s decision to make nurse staffing a National Performance Goal represents a major healthcare staffing industry change with far-reaching effects for hospitals, nurses, and patients. By emphasizing the importance of adequate staffing, this update encourages healthcare facilities to prioritize recruitment and retention, creating more opportunities for nursing professionals and supporting a stronger, more capable workforce.
When hospital workforce management is approached strategically, facilities can better comply with Joint Commission standards while improving overall care quality. This includes:
- Leveraging per-diem staffing models: Bringing in skilled nurses on a flexible basis ensures that patient needs are consistently met, even during peak times or unexpected absences.
- Enhancing workforce efficiency: Implementing healthcare staffing automation and technology tools allows for smarter scheduling, streamlined workflows, and optimized resource allocation.
- Supporting nurse satisfaction and retention: Adequate staffing reduces burnout, improves job satisfaction, and helps retain top talent, creating a more stable and experienced workforce.
Ultimately, these changes are not just about compliance, they reflect a broader healthcare staffing transformation, where technology, flexible staffing strategies, and data-driven workforce management come together to improve both patient outcomes and the working conditions for nurses. By embracing these strategies, healthcare organizations can foster a culture of excellence, resilience, and positive change across the industry.